My Breast Cancer Journey

Being diagnosed with invasive lobular breast cancer once rocks your world in a way that is hard to imagine. But making it through my breast cancer journey initially and then finding another lump just a year and a half later in the other breast that is yet again invasive breast cancer… this time they ductal variety… it is enough to make you question everything. The only sense I can make of this second diagnosis is that I am supposed to share my story with the world. God has filled me with a sense of urgency that I need to help others find breast cancer before it spreads.
Through sharing my story, I pray that you have three primary take aways…
#1. You have to be your own health advocate. BOTH times, I found the tumors in my breast though self breast exams and pushed to have them biopsied after mammograms and ultrasounds.
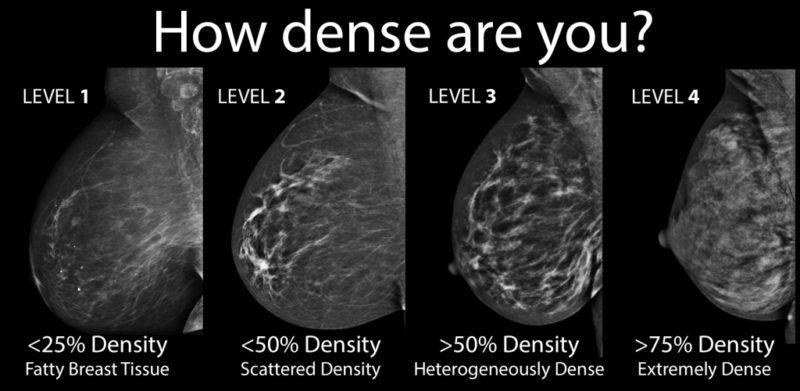
#2. Self breast exams in addition to diagnostic tools like Mammograms HAVE to be a regular part of your life, especially if you have a family history &/or dense breast tissue. For me personally with extremely dense breast tissue, mammograms where white outs which means that it was impossible to see any abnormalities with them. Following mammograms up immediately with ultrasound was the only way to visualize the lumps that I saw and it took a biopsy to appropriately classify the lumps and cancerous tumors.
#3. Breast cancer is a very treatable disease. Finding it early makes a HUGE difference in the outcome. DO NOT PUT OFF ROUTINE TESTING. 5 year survival rates for breast cancer that has not spread to the lymph nodes is 98%.
Listen to the Podcast Episode
My Breast Cancer Journey Begins
After a year and a half of following a palpable lump in my left breast with mammograms and ultrasounds, I pushed to have the small lump that I could feel biopsied. When the results came back that I did indeed have breast cancer, it took time to process everything. Below are some of the steps that I went through in this process.
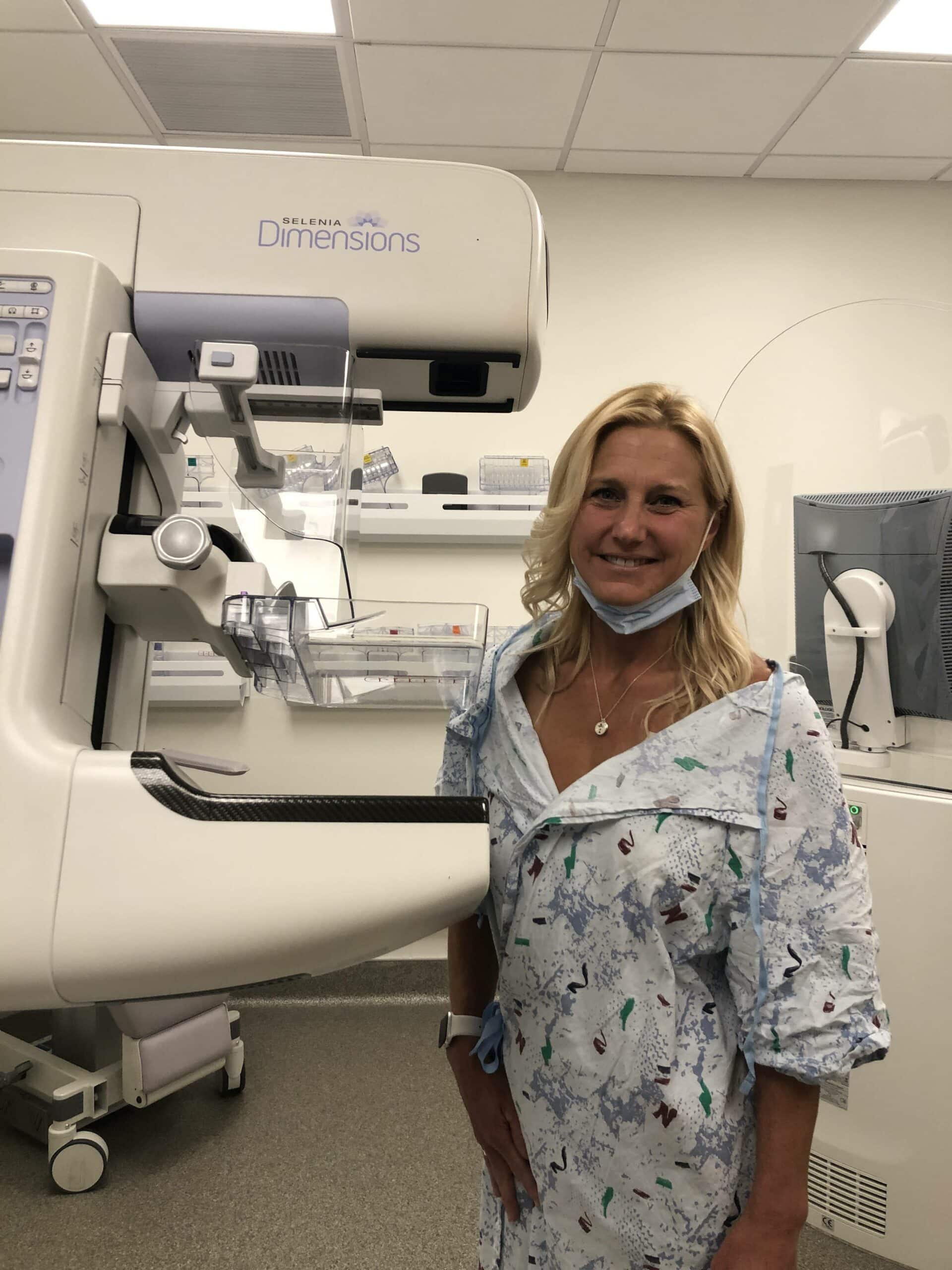


My Breast Cancer Journey – Imaging beyond mammograms | Breast MRI & Genetic testing for breast cancer | BRCA testing
The next step after my initial biopsy results was a breast MRI to more fully image the cancer and to see if there were other spots of concern. I did end up having a second 5 cm area that was concerning and I was immediately sent for a second biopsy. Luckily that ended up being a large, fluid filled cyst… benign. It was determined that we were indeed just dealing with one tumor.
I was also sent for genetic testing to see if I carry the BRCA I or BRCA 2 genes. These are the genes most commonly affected in hereditary breast and ovarian cancer. Less than 10% of all breast cancers result from inherited mutations in the BRCA1 and BRCA2 genes. That is right… less than 10%! I am BRCA negative and have very limited family history. While we may never know the root cause of my breast cancers, it does not appear to be related to those genes.
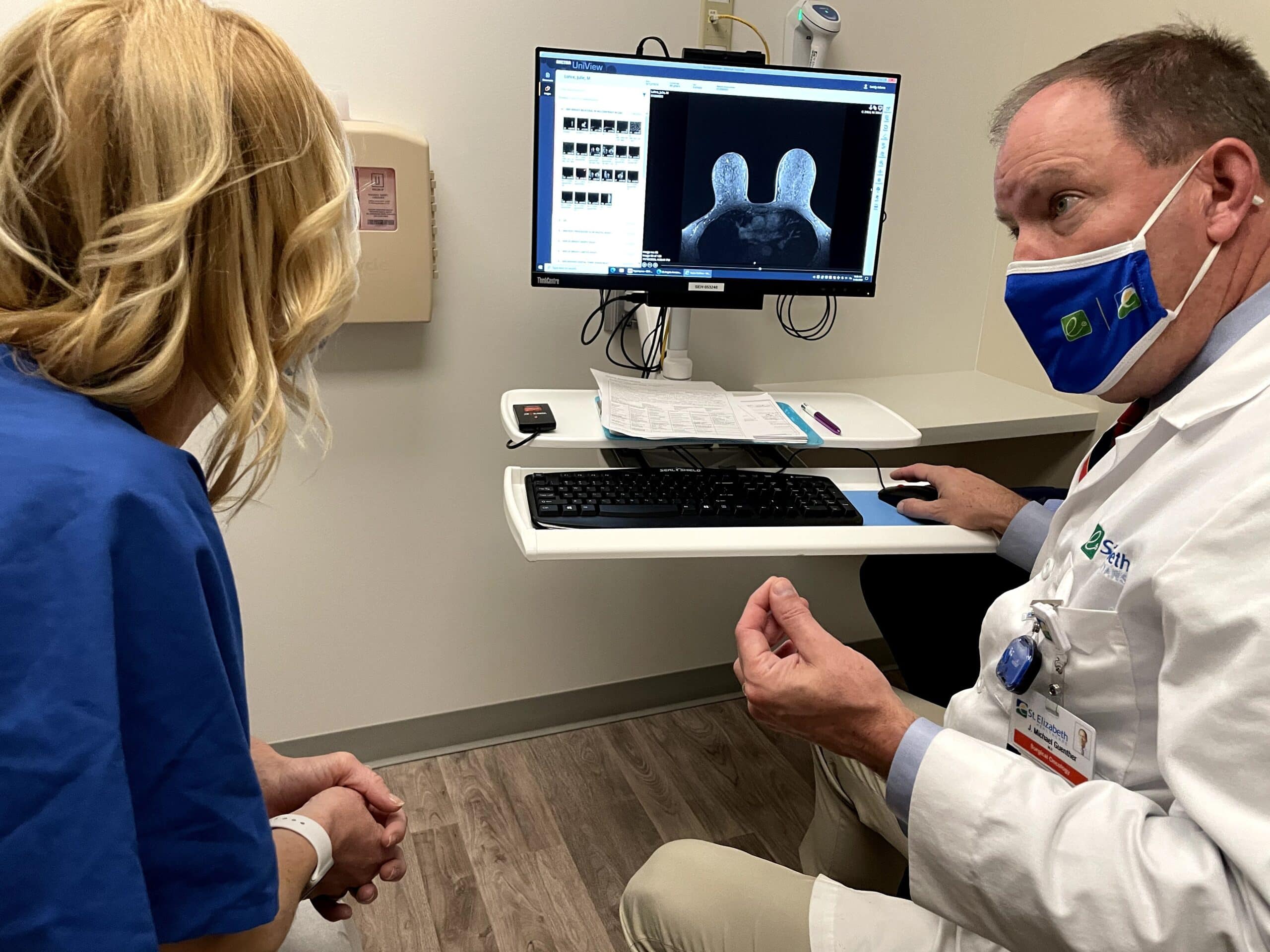
Breast Conserving Treatment – Lumpectomy with Radiation on my Right Breast
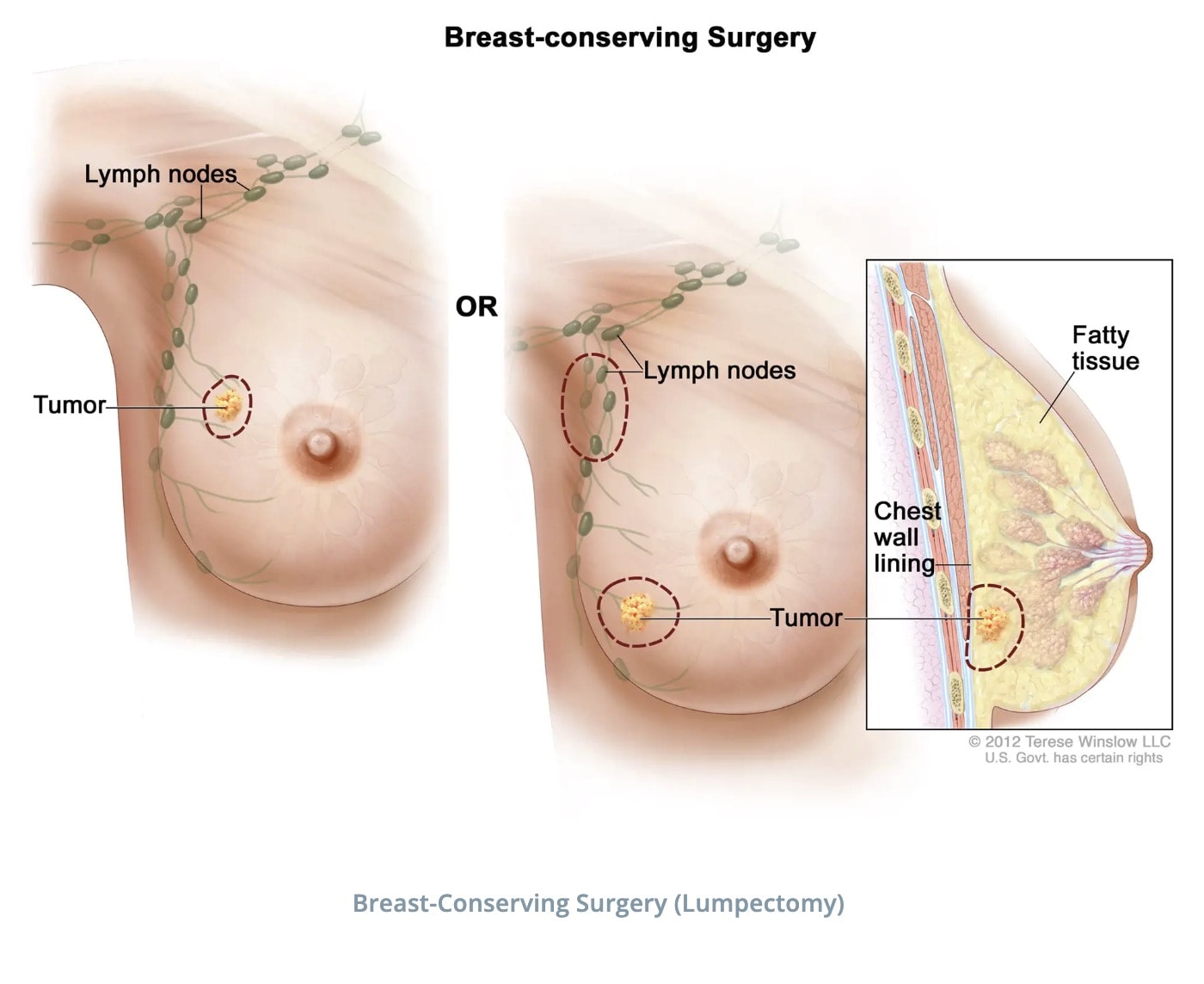
My Breast Cancer Journey – Tumor removal through lumpectomy.
After extensive consults with doctors and doing lots of research on my own, I choose to have a lumpectomy with sentinel node biopsy, followed by radiation to excise the invasive lobular carcinoma and to irradiate any cells that might have been missed in surgery. Interestingly when the tumor was removed it actually measured double what it was thought to be on ultrasound. Instead of a really tiny 7-8 mm mass, the invasive lobular cancer had spread out – as lobular cancer often does.
Still stage one, the tumor ended up being 1.6 cm. The node biopsy was negative which means that they did not detect any cancer cells in my lymph nodes. At this point, the biggest question was whether or not I would need chemotherapy. I am so fortunate for the advances that have happened in breast cancer research! If I had been diagnosed 10 years ago, I would have certainly been sent for chemotherapy along with surgery and radiation given my age of diagnosis.

Immediately from surgery, samples from my tumor were sent off for further testing. My doctors utilized the Oncotype DX test which is a specialized genomic test that examines a sample of a breast cancer tumor to determine the activity of a group of genes. By analyzing these genes, the test provides insights into how likely it is that the cancer will return within 10 years after initial treatment and how beneficial chemotherapy might be for preventing that recurrence.
The results of the test are given as a score ranging from 0 to 100. Mine came back at a 16 which suggested a moderate risk of recurrence. Scores below 18 have indicated that the benefits of chemotherapy are likely limited, so patients may not significantly benefit from adding chemotherapy to their treatment plan. This saved me from the potential side effects of chemo while still effectively treating the cancer with other therapies like hormone therapy.
Recovery from my surgery took about 2-3 weeks during which time I did a lot of resting but was still able to work through email. One of the benefits of working from home for yourself. I did develop a large seroma under my arm at the site of the sentinel node biopsy which bothered the crap out of my while I tried to type. That lasted for about a month and was drained twice. Eventually that went away. After this, I began radiation therapy.

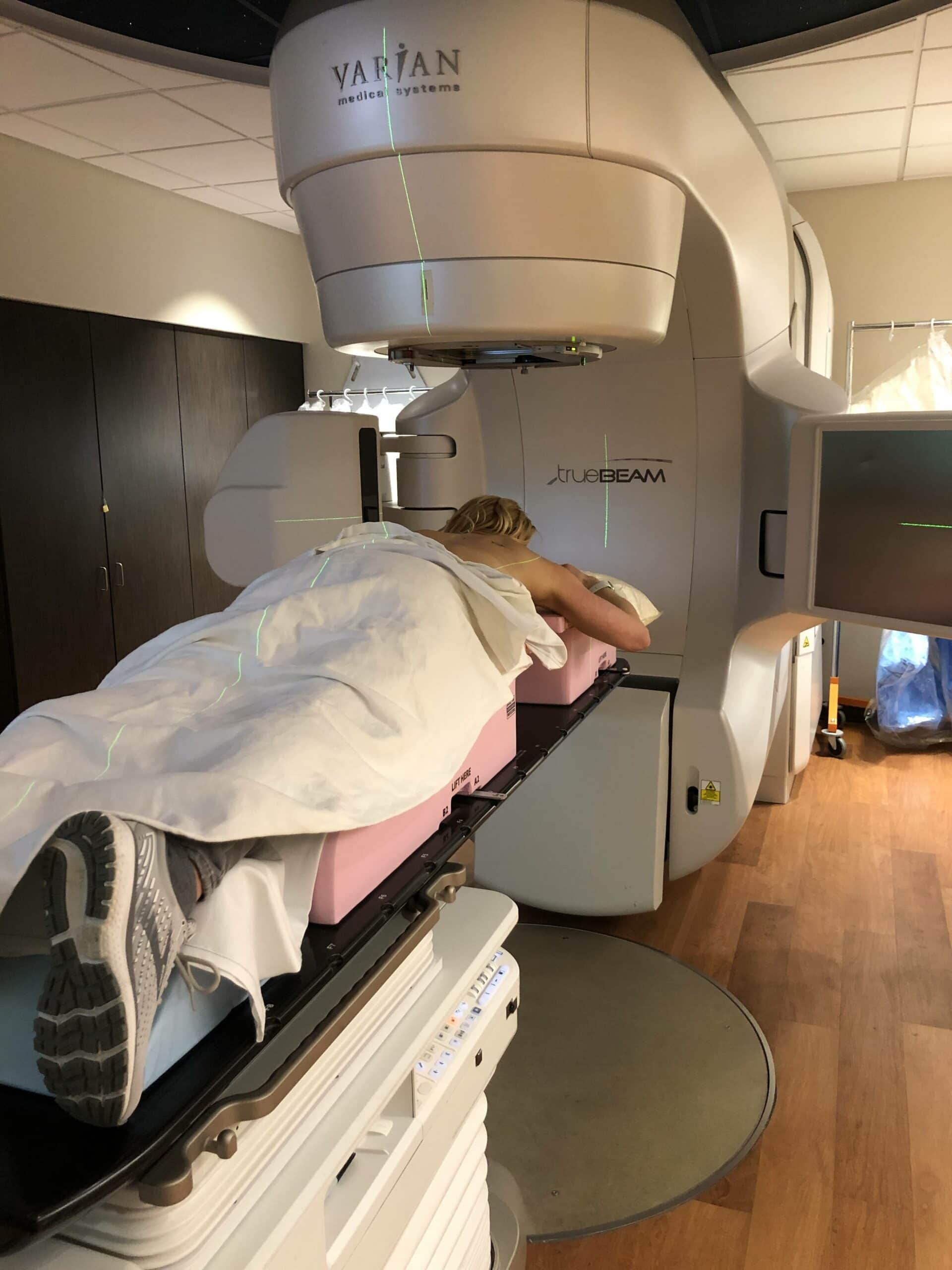
My Breast Cancer Journey – Radiation Therapy
As part of the breast conserving treatment, lumpectomies are matched with radiation to eliminate any rogue cancer cells that could be in the tissue surrounding the tumor. Radiation therapy took 1 month in total and I visited the hospital Monday – Friday each day for the 30-45 min sessions. The radiation therapy itself only takes about 10-15 mins. 16 sessions were for whole breast radiation, with an additional 4 sessions specifically targeted to the area where my invasive cancer had occurred. The sessions are totally pain free. That said, there are side effects from radiation therapy. I experience short term side effects of fatigue, nausea, reddening of the skin / burns, some modest blistering and heat. Those subsided within a month or so after my treatment.
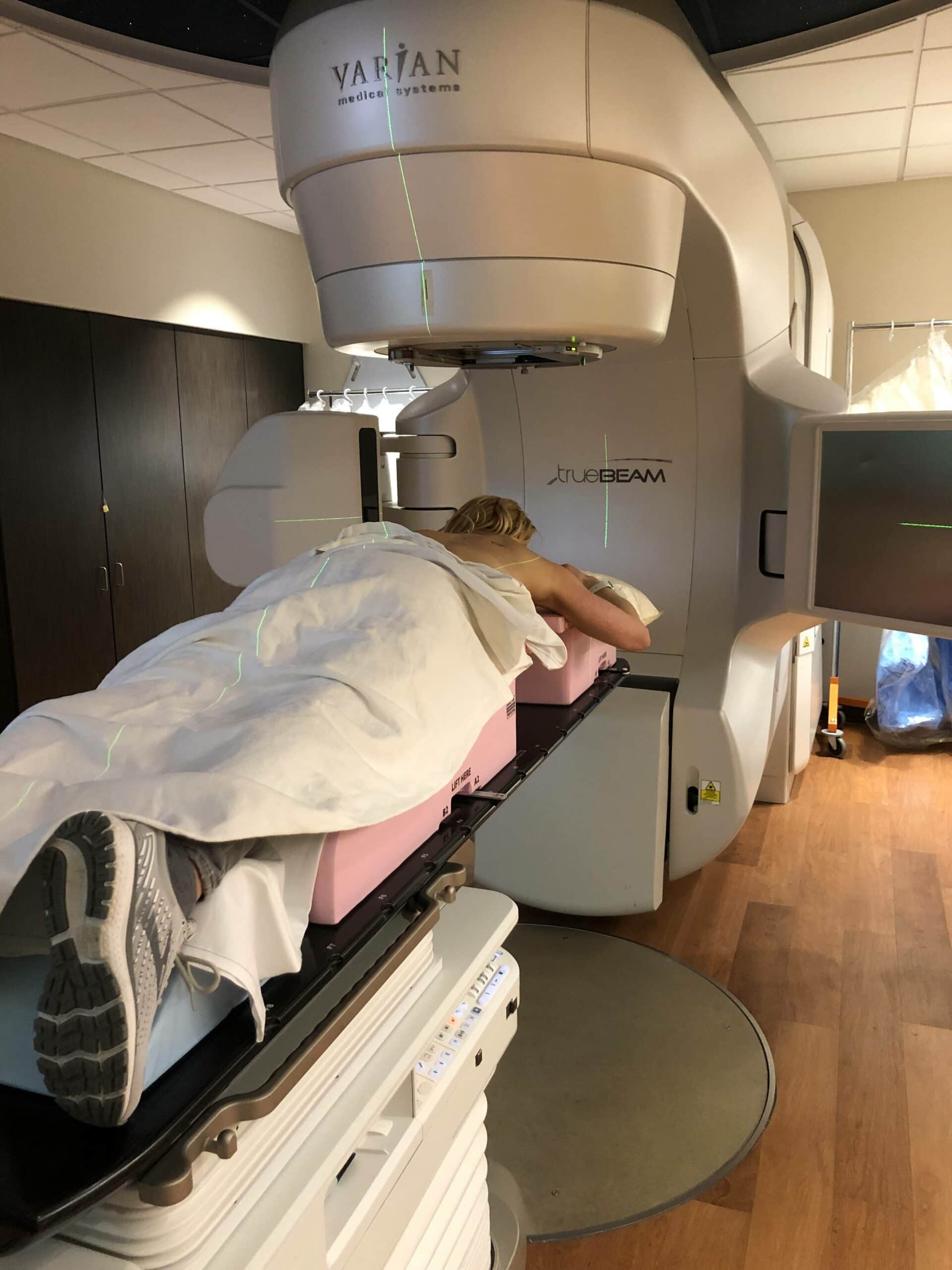
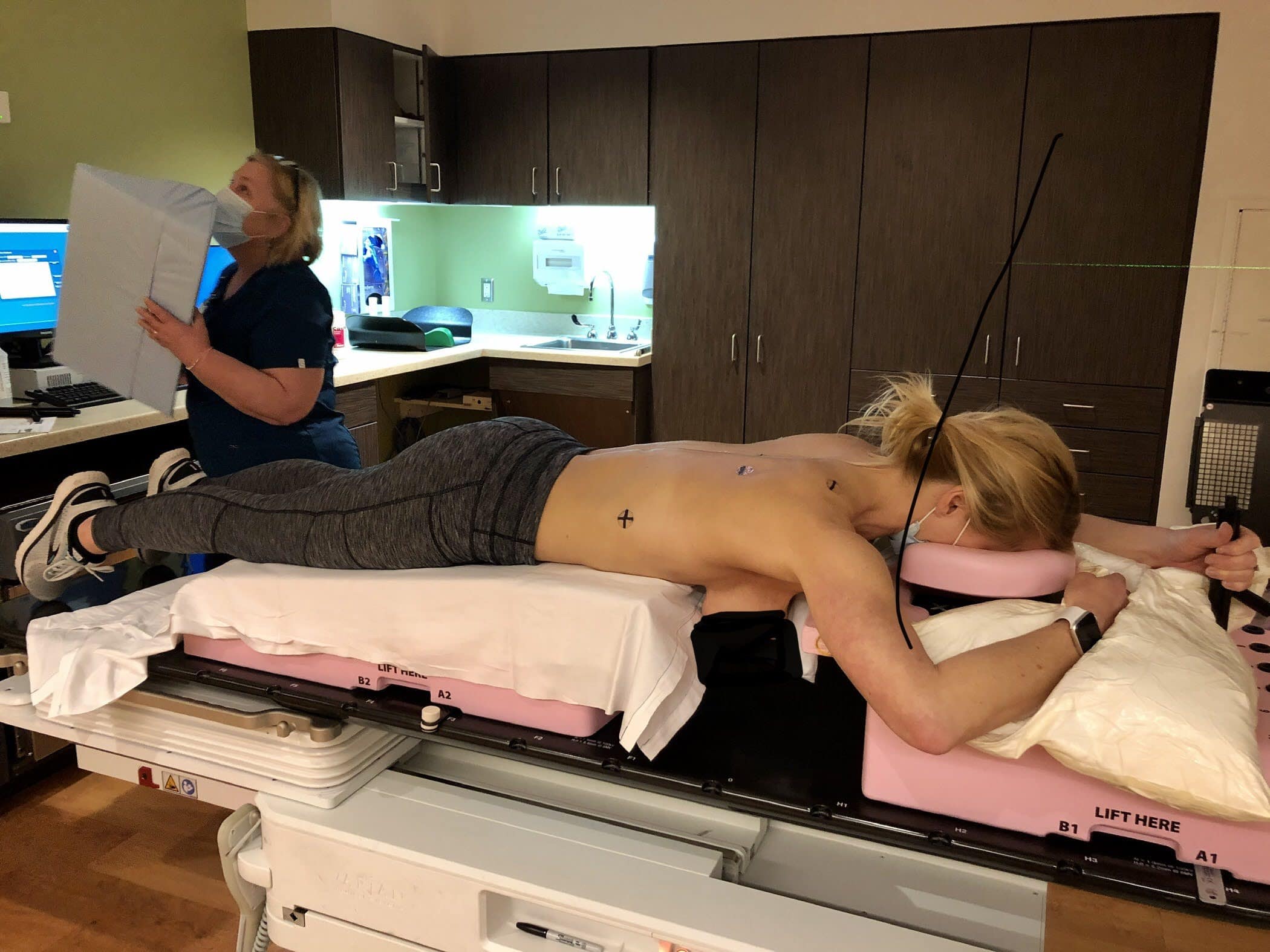
My Breast Cancer Journey Next Steps – Hormone Therapy with Tamoxifen & Anastrozole for Breast Cancer
When you are diagnosed with hormone positive breast cancer, that means that the tumor cells respond and grow under the influence of estrogen, progesterone, or both. My initial lobular carcinoma was estrogen and progesterone positive. While the tumor was removed and there were no obvious signs of cancer spread through my lymph nodes, there is always the possibility that microscope clusters or individual cells could have escaped to other areas in my body.
When those cells do escape they tend to head to areas like the bones or brain and begin setting up shop. This is called metastatic breast cancer. The interesting thing is that those cells are still breast cells are heart and still respond to hormones. So, the standard treatment is to either block the estrogen receptors on breast cells through a medication called tamoxifen for pre-menopausal women or to decrease the amount of estrogen the body makes and helps to slow or reverse the growth of these breast cancers through aromatase inhibitors like anastrozole.
I started with Tamoxifen but had significant side effects that made it difficult for me to continue including severe headaches and mood changes, along with uterine changes and concerns. Looking back, I wish I had pushed through those initial challenges with tamoxifen because with my second time around, those did get better. I will always wonder if my second primary breast cancer would have occurred if I had just sucked it up and taken the tamoxifen as prescribed. Hindsight is 20:20, right?
Since my surgery and treatments, I officially entered menopause fairly early (47). For the last year or so, my estrogen and testosterone levels come in at zero. Good for avoiding breast cancer recurrence but I do struggle with the impact of having no hormones and not being able to utilize hormone replacement therapy.
My Breast Cancer Journey – Life after invasive breast cancer treatment… the worry is real.
Following my initial diagnosis and treatment, life went back to normal… mostly. The dr visits went from weekly to every 6 months. I started a more intense monitoring schedule for my overall breast health with mammograms yearly alternating in with Breast MRI’s every 6 months.
The uneasiness that comes after being diagnosed and following my breast cancer journey is a challenge to live with. While recurrence remains rare, it is most likely to happen in the first 5 years and women that have had breast cancer before are at higher risk of having it again. This is always in the back of your mind. I continued with self breast exams every 2 weeks or so (month is recommended) and would occasionally find new lumps and bumps that scared the heck out of me. While breast conserving surgery for breast cancer is highly effective, it does not take into account the psychological impact that living with the breasts that had betrayed you has on your psyche.
Looking back, I wish I had gone forward with a double mastectomy to start for a number of reasons. But I will get into that more in part two… Invasive Breast Cancer – Take 2
Click here for my second journey with breast cancer





